| O2 BLOOD in Vol.% | 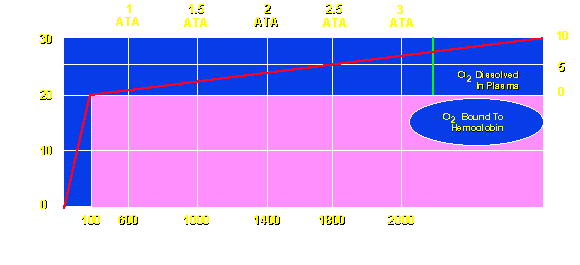 |
pa02 in mm Hg |
OVERVIEW OF HYPERBARIC MEDICINE |
Since the late 1960’s the USAF has been actively involved in advancing the science of
Hyperbaric Medicine. An initial contributing factor to this advancement of knowledge
regarding hyperbaric therapy was associated with the need to address the issues of
prevention and treatment of altitude-induced decompression sickness in military aviators.
Treatment with Hyperbaric Oxygen (HBO2) had just broached the horizon with the landmark
case of aviation related neurological DCS successfully treated with HBO2 reported in 1959.
A chamber complex was created at Brooks AFB, Texas to investigate this new treatment
modality. Not only did subsequent studies validate HBO use in altitude-induced
decompression sickness, but also suggested its benefit in other medical maladies.
Early Air Force investigators — Jefferson Davis, Dean Heimbach, Jared Dunn, and Paul Sheffield — set the stage for reviving interest in Clinical Hyperbaric Medicine in America. Prior to their work, Hyperbaric Medicine was an "outcast" from mainstream medicine. This was the result of very public charlatanism in the 1920’s and 1930’s. The work that these USAF clinicians and researchers produced created the foundation upon which modern Hyperbaric Medicine has grown. Their work eventually resulted in the creation of the USAF Clinical Hyperbaric Medicine Program in 1974. In the ensuing years it became clear that decompression sickness was no longer the sole disease entity for which HBO was effective. The US Air Force was now leading the way in Clinical Hyperbaric Medicine. In fact, in 1984, the Department of Defense named the USAF Program its Lead Agent for Clinical Hyperbaric Medicine. PresentlyMedicine.Presently, Davis Hyperbaric Laboratory (DHL), named for the late Jefferson Davis, remains at the forefront of Air Force and Department of Defense Hyperbaric Medicine.
During these "red letter" years the education of new generations of Hyperbaric Medicine specialists was specifically addressed through introductory science courses. The early 1980’s further saw the inception of numerous training courses. Training of enlisted operations technicians and medical technicians was organized. An in-depth course for nurses was also created. A nine-month Physiology Fellowship was developed, but is no longer conducted. And, a formal one year physician Fellowship was designed and implemented. This assured a continuous flow of quality trained personnel to staff the USAF Clinical Hyperbaric Facilities at Brooks AFB (Texas), Travis AFB (California), and Wright-Patterson AFB (Ohio). This education mission continues today as a major thrust of the USAF Clinical Hyperbaric Medicine.
From this modest beginning, modern HBO has become a widely accepted treatment modality. The basis for its effectiveness, of course, lies in the delivery of oxygen in excess of basal metabolic needs of the tissues, i.e., use of oxygen as a drug in what might be considered a pharmacological dose. Normally, the red blood cell mass and plasma carry about 20 vol % (20 ml O2/100 ml blood) oxygen. At sea level the vast bulk of oxygen is carried by the hemoglobin molecule. By delivering 100% oxygen at 3 ATA (66 feet sea water equivalent pressure) another 6 vol % oxygen can be dissolved in the plasma. Since only 5-6 vol % oxygen is necessary to support aerobic metabolism of the body, HBO (i.e., oxygen dissolved in the water portion of the blood) and plasma alone can sustain life—were it necessary (see Figure below). In fact, Boerema et al. were able to demonstrate that with a piglet model.
| O2 BLOOD in Vol.% |  |
pa02 in mm Hg |
In order to treat with HBO, patients must enter a hyperbaric pressure chamber. Traditionally, this has been a multiplace chamber. However, the last several years have seen a rapid rise in monoplace chamber use. Although the monoplace chamber is less costly and more mobile, its atmosphere is often pure oxygen (an increased explosive fire risk), and there is no "hands-on" capability. In contrast, the multiplace chamber has been expensive to install, is not mobile, yet has an air atmosphere which diminishes fire risk (oxygen is delivered by mask or hood), and requires an inside attendant—which enables patient access for all routine and emergency care. A recent facility census suggests that at least 160 multiplace chambers and 450 monoplace chambers are in use throughout the USA and Canada.
With this proliferation of HBO treatment chambers, the Undersea & Hyperbaric Medical Society (UHMS) has taken the lead in Hyperbaric Medicine. Initially founded to nurture the science of Diving Medicine, the UHMS subsequently embraced Hyperbaric Medicine. Due to the historical perceptions of quackery, the UHMS (in 1976) created a standing committee to rigorously examine the indications for HBO. It examined physiologic principles, theoretical possibilities, treatment experience, case reports, animal models, patient-matched research protocols, and double-blind controlled studies. Since its first formal committee report in 1976, the committee has continued to issue a routine review of the world’s literature about every 3 years. The 1999 report lists 13 approved indications for HBO (See the Table below).
|
Secondary (adjunctive)
|
|---|
As mentioned previously, the primary mechanism of action for HBO is an excess, or overabundance of oxygen delivery to the tissues. This extra oxygen is carried by the plasma. Within a hypoxic tissue bed there are severe impediments to healing. Not the least is a lack of a steep oxygen gradient between wound and periphery, i.e., inadequate diffusion gradient for oxygen. Without such a gradient, healing is not initiated or is minimally successful due to the hypoxic wound site. Hypoxia (PO2 less than 30-40 mmHg) impairs the function of both leukocytes and fibroblasts. Neither cell is effective. The leukocyte is unable to effect oxidative bacterial killing and the fibroblast is unable to produce collagen. The result is a wound devoid of new collagen (and, thus, granulation tissue), an inadequate matrix for restructuring the tissue, and an tissue site frequently infected with a significant bacterial population. This is obviously not a favorable healing environment.
Of particular note are the problems associated with radiation tissue damage. The chronic progressive vascular changes result in hypovascular, hypoxic, and hypocellular tissue. This predisposes the tissue to breakdown with subsequent nonhealing of the irradiated tissue. HBO has been shown to recreate the milieu whereby angiogenesis can occur. In fact, Marx et al. noted an increased neovascularization to 75-85% of normal. This effect was produced using 30 treatments. In addition, the neovascularization persisted for at least 7-8 years. With the advent of HBO treatment in this disease entity, the surgical treatment of mandibular osteoradionecrosis has undergone a complete turn of events—with dramatic results! Instead of a 92% failure rate, it is now 92% successful. As a result, the National Cancer Institute in a recent consensus statement declared HBO the "standard of care" for mandibular osteoradionecrosis. In light of this medical experience, any surgery within a significantly irradiated tissue field may well be considered for preoperative HBO.
Another area of intense interest for HBO therapy is reperfusion injury. Following a period of ischemia and anaerobic metabolism, hypoxic tissue eventually undergoes reperfusion. Examples include crush injury, compartment syndrome, skin grafts, composite flaps, acute arterial insufficiency, myocardial infarction, stroke, and burns. The critical adversity associated with the initiation and acceleration of this reperfusion injury phenomenon is neutrophil activation and adhesion to endothelial surfaces. Subsequently, there is a progressive free radical production and release by these neutrophils that results in increased tissue damage and eventually the "no reflow" phenomenon. At this point, the affected tissues die. Zamboni et al. have discovered that HBO mitigates the neutrophil adherence and thereby attenuates the degree of reperfusion injury. Needless to say, this is a very exciting and active area of research.
There are numerous other physiologic bases for the use of HBO. The following Table enumerates many of them:
| CATEGORY | HBO INDICATION | HBO MECHANISM |
| Infection | clostridial gas gangrene necrotizing fasciitis refractory osteomyelitis intracranial abscess |
halts alpha toxin production direct antibacterial activity antibiotic synergism increased neutrophil oxidative killing increased osteoclast activity decreased hypoxia increased oxygen diffusion distance |
| Reperfusion | compromised skin grafts/flaps crush injury/other acute ischemias acute thermal burns |
decreased fluid requirements decreased
edema formation increased ATP levels increased superoxide dismutase levels increased red cell deformability decreased platelet aggregation vasoconstriction inhibited neutrophil adhesion/activation decreased hypoxia increased oxygen diffusion distance |
| Wound Healing |
osteoradionecrosis -soft tissue radionecrosis selected problem wounds -vascular insufficiency -diabetic ulcers |
ecreates steep wound hypoxic gradient increased fibroblast activity increased collagen deposition increased angiogenesis decreased hypoxia increased oxygen diffusion distance |
Furthermore, the following Chart diagrams the interrelationships of these mechanisms in a simplified fashion.
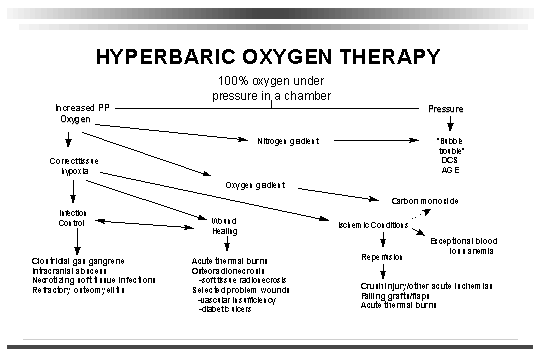 |
Treatment in a hyperbaric chamber does not occur without risk. The most commonly encountered hazard is barotrauma, and the ear is the most frequent site. Here the descent-induced middle ear negative pressure can result in pain and eardrum damage (even to the point of rupture). This problem is avoided by generous application of "clearing" maneuvers (i.e., Valsalva, Frenzel, and Toynbee maneuvers). Likewise, sinus problems can occur; however, these are much less common.
Since HBO is the administration of oxygen in a pharmacological dose, side effects are possible. Oxygen toxicity can occur. Although many different organ systems can be affected, the brain and lung are of greatest clinical significance. CNS toxicity is manifested by visual disturbances, auditory hallucinations, nausea, facial twitching, irritability, and dizziness. Most impressive is the rare tonic-clonic seizure. It is without sequelae. The reported seizure incidence here at DHL is 1 per 10,000 treatments. Pulmonary toxicity is generally without clinical significance, however, treatment of complex cases of decompression sickness can sometimes generate this complication.
Diabetic hypoglycemia, temporary myopia, and ulnar paresthesias also occur. The etiologies are unclear. And, finally, claustrophobia is occasionally seen.
Each year here at Davis Hyperbaric Laboratory approximately 250 patients are evaluated and treated and over 3000 treatments are prescribed. To date in excess of 5,000 patients have been treated. DHL has three multiplace chambers and one monoplace chamber. A twelve-place chamber is typically used for the majority of our patient care. The four-place "Panama" chamber (probably the oldest operating hyperbaric chamber in the USA, dating back to 1903-1904) is available for patient overflow and customizing of treatment protocols. We also have a Sechrist monoplace chamber which can be utilized. Most of the patients are referred from three tertiary care hospitals (Audie Murphy VA Hospital, USAF Wilford Hall Medical Center, and Brooke Army Medical Center).
This large patient population forms the foundation for the USAF Physician Fellowship in Clinical Hyperbaric Medicine. This is a broad-based intense study of Hyperbaric and Hypobaric Physiology, Wound Physiology, Diving Medicine, and Clinical Hyperbaric Medicine. The duration of study is one year. Prospective Fellows are expected to be board eligible/certified in a Primary Care or Surgical Specialty. In addition, each Fellow must be a Flight Surgeon having completed the USAF Aerospace Medicine Primary Course or its equivalent. Responsibilities during the Fellowship include patient care, formal lectures, conference presentations, research, USAF Hyperbaric Newsletter articles, a structured reading program, and multiple outside courses and rotations designed to enhance and supplement their DHL experience. The final product of this Fellowship is a physician who is among the finest trained operational Hyperbaric Medicine specialists in the country.
Air Force Hyperbaric Medicine is not limited to Brooks AFB. Since its dedication in March 1986, the Wright-Patterson AFB Unit has treated over 1200 patients, averaging 27 treatment dives a month (Note: this facility has transitioned to contractor operation in Oct 99). In addition, the Travis AFB Unit, which opened its doors in November of 1990 averages 44 treatment dives monthly. The Travis facility is staffed by physicians who have received specialized USAF Fellowship training in Hyperbaric Medicine.
In summary, Clinical Hyperbaric Medicine is a rapidly growing medical specialty. The basis for wound care and hyperbaric oxygen therapy are grounded in sound physiology. Research is consistently unearthing hidden mechanisms that were unpredictable or unexpected (i.e., reperfusion injury mitigation). Research and patient care experiences at the Davis Hyperbaric Laboratory were instrumental in the revival of Hyperbaric Medicine. Today, DHL remains at the forefront of Clinical Hyperbaric Medicine and is considered by many to be the birthplace of modern Hyperbaric Medicine. The present training curriculums are well-structured, intense, and innovative. Whether for the technician, nurse, or physician, there is no better recognized program than that found here at the Brooks AFB. In fact, the physicians Clinical Hyperbaric Medicine Fellowship is the "model" to be copied.